Using a laboratory for water analysis of bacteria (microbiology)
From our experts at SimplexHealth
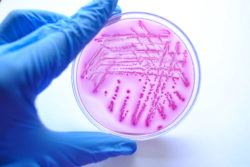
Often customers ask us about the differences in the various types of bacteria analysis available and what the results mean for them. Testing bacteria using laboratory analysis are important tests and necessary for effective water quality monitoring. Different types of bacteria identified can provide information on the causes of pollution and how water should to be treated.
Generally, bacteria grow most in warm environments and temperatures, like hot tubs, hot water tanks & pipes and this is where the risk for human health is greatest.
Bacteria are mostly measured in cfu (= colony forming units) in the sample volume measured (ie. 100ml) and results are presented in cfu/100ml or cfu/ml.
In the lab, special techniques are used to encourage the bacteria to grow and multiply in the sample. The colonies which have grown are then identified, measured and quantified to provide a meaningful result.
Below you will find some further explanations for each type of bacteria analysis, which should help pick the correct bacteria testing for your requirements.
Coliform/E.coli:
This is the most important routine check on drinking water. Coliform bacteria is a group of bacteria which includes E.coli, Klebsiella, Enterobacter and Citrobacter. These bacteria are mainly of faecal origin and give an indication of the water quality of potable water. Whilst coliforms can naturally occur in soil and plants, it is worth noting that E.coli does not grow in water, E.coli can only get into water from faeces of humans or animals, therefore it is important part of the water testing process.
–> Should be tested regularly in drinking water, swimming pools and open water for public swimming. Can be used to test for sewage spills after flooding or in rivers and lakes.
In drinking water the amount of coliform and E.coli should be zero. In pool water they should also be absent. For open water swimming (in lakes & rivers), the level should be no greater than 500cfu/100ml to achieve an excellent grade.
Enterococci:
Commonly found in the faeces of human and warm-blooded animals. Enterococci testing is used to check for faecal contamination in water (like fresh, marine, drinking and waste water) – it is an indicator of faecal pollution and possible enteric pathogens.
–> Should be tested regularly in drinking water as well as open water for public swimming. Can be used to test for sewage spills after flooding or in rivers and lakes.
In drinking water the result should be zero. For open water swimming, a result of up to 200cfu/100ml is required for an excellent grade.
Total Viable Count (TVC) / Aerobic colony count:
This is a basic measurement of the total amount of microorganisms, like bacteria, yeast and mould species, in a water sample. It is measured by leaving the sample plate at a temperature of 22°C and 37°C for 48 and 72 hours (22°C mimics the ambient water temperature and 37°C the body temperature of humans.)
–> It is a useful test for regular maintenance of most water systems. It is recommended to carry this test out regularly, this will give a baseline measurement and help identify sudden increases/changes and any potential problems early. For example, in pool water and hot tubs regular testing provides guidance to whether the filtration and disinfection systems are working well. In pool water results should be less than 100cfu/ml and consistently high colony counts should be investigated.
There is no strict regulation for an acceptable level of TVC in drinking water. The guidelines state that there should not be a high count and there should be no significant increase from an incoming water supply.
Pseudomonas aeruginosa (P.a.):
Is a rod-shaped bacterium and is the one type of pseudomonas bacteria which most often causes infections in humans. It is commonly found in the environment like water and soil or on damp surfaces (subsequently forming a biofilm). It is a pathogen which is capable of growing in water, even at low temperatures. An infection in a healthy individual is rare but it can seriously affect people who are immuno-compromised. P. aeruginosa can cause skin rashes and ear infections, even in healthy people. Infection in buildings/households often comes from bacteria build up (biofilms) around faucets, showerheads and similar. In pools they can colonise transfer channels, filters, pool covers, swimming aids, etc.
–> Organisations have a legal obligation to assess the risk for humans, especially in pool & hospital environments and other places where humas regularly come in contact with water.
Should be tested regularly in swimming pools and hot tubs, P.a. should be zero in a 100ml sample. If the count is between 10cfu/100cl and 50cfu/100ml the sampling and analysis should be repeated. For counts above 50cfu/100ml pool closure is advised to reduce the risk for bathers. Routine testing of P. aeruginosa in mains water is not required. Often the presence of Pseudomonas in drinking water is not a problem, but when growth is sufficient it will lead to a deterioration in water quality, unacceptable taste and odour. In such cases P. aeruginosa should be ruled out as a cause.
Clostridium perfringens (C. perfringens):
C. perfringens are found in water, soil and the intestinal tracts of humans and warm-blooded animals and can cause a variety of illnesses, therefore its presence in water is an indication of faecal contamination in the water supply. Clostridia are a group of bacteria that are very long lasting and resistant to harsh conditions, including the methods often used to disinfect water. When they are found in water samples it can be a sign that, although any disinfection process may be working effectively, the supply may have been contaminated in the past. It may also mean that any filtration process is not working effectively and the supply may be at risk from the organism known as Cryptosporidium, which can cause illness. There is a requirement in England, Wales and Scotland to test for C. perfringens in private water supplies. The presence in drinking water should be zero.
Legionella bacteria can cause the serious illness of legionnaires disease. A detailed resource on Legionella causes/ risks/ testing can be found here.
Check below to view microbiological / bacteria laboratory tests:
- To test potable/drinking water
- To test water from lakes & rivers
- For open water swimming testing
- For pool and hot tub testing
- To identify pollution from sewage (=faecal bacteria) in rivers or after flooding
- Monitoring bacteria in hot tubs & pools
Disclaimer: All guidelines and recommendations accurate at time of publishing. Please check current regional / local guidelines relevant to your situation. We can not be held responsible for any information published on this webpage. Only opinions based upon our own personal experience or information available in the public domain is cited. This has been done exclusively for anyone who is interested in this subject but is not intended to replace proper research & analysis. We cannot accept responsibility and liability of any kind which may result from the application of this information. We always recommend to consult an expert to discuss any test results or get a full recommendation on the specific subject and specific to your situation by an expert. We also recommend to check if there is any newer or later information on this subject.
This information is owned by SimplexHealth and you do NOT have the right to reprint, sell, auction or distribute this information.
